For those of you who have ever read a research article and thought it was a tough read, i’d like to let you in on a little secret. Doing the research is far worse! If only memes were a thing when I started my Masters of Applied Science thesis, I’d have changed my background to remind myself that conducting research was even drier than every dish an apprentice has cooked for Gordon Ramsey.
My mentor at the time, who was the manager of the sports science and sports medicine devision of Cricket Australia and later the head of the AIS human movements department, Dr Marc Portus, enlightened me with something quite profound. He said, “There are two outcomes from a thesis. Either you live it for the rest of you academic days or it sits on a bookshelf for years collecting dust.” Given I completed my thesis and went straight onto my graduate entry physiotherapy masters, it is fair to say i’m in the later camp. Quite a few years have passed now however, so I’d thought i’d dust off the cover and summarise my thesis for all of you playing at home!
So not to degrade my self entirely, I thought I found some pretty good stuff that has affected the way I assess and treat today. I haven’t shared it all today as it was more than 140 pages long and ‘ain’t nobody got time for that’. More importantly though, my thesis reminded me of the passion I have for lower limb biomechanics and that physiotherapy (as opposed to research) was always meant to be on the cards for me. My thesis, “The 3D Kinematics of the Single Leg Flat and Decline Squats” boiled down to looking at how the ankle position changed the joint angles single leg squat, how hip strength affected the squat as well as few other things that aren’t worth mentioning here.
BACKGROUND:
The single leg squat (SLS) replicates an athletic position commonly assumed in sport such as cutting (powerful change in direction while running made from one leg), jumping and balancing which all require the control of the trunk and pelvis on the weight bearing femur in all three planes of movement [1-5].


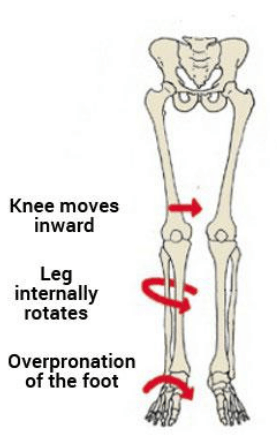
As such, the SLS is commonly used by clinicians as a functional measure of dynamic lumbo-pelvic stability [endif]–[6-8]. Abnormal movement within the SLS tend to be characterised by the commonly described “medial collapse” or “dynamic valgus”. Specifically, there is excessive femoral internal rotation, femoral adduction, knee valgus, tibial internal rotation and foot pronation of the weight-bearing limb with resultant excursion of the contralateral non weight bearing Ilium and excessive lateral flexion of the trunk [endif]–[3, 6-8].
The reason why this tends to be perceived as a big deal is that this position tends to be argued as a lack of lumbopelvic stability and results in increased loading of the knee. Moreover, pelvis weakness tends to be ascribed to the absence of stability ultimately resulting in a position in which many acute and overuse injuries of the lower limb may occur. These ailments include, ACL / MCL ruptures, patellofemoral pain syndrome (PFPS), illiotibial band friction syndrome (ITBFS) and shin splints to name a few. That is why the SLS appears to be a valuable rough screening tool in clinical practice.
MY FINDINGS:
As mentioned, I looked at how a decline board of 20 degrees changed the angles of the lower limb during the squat. I also looked at if any strength measures of the hip related to how someone squatted between conditions. Finally, I looked at if the decline board altered how someone was scored by experienced physiotherapist as a competent or not at the squat
JOINT ANGLES (KINETMATICS:)
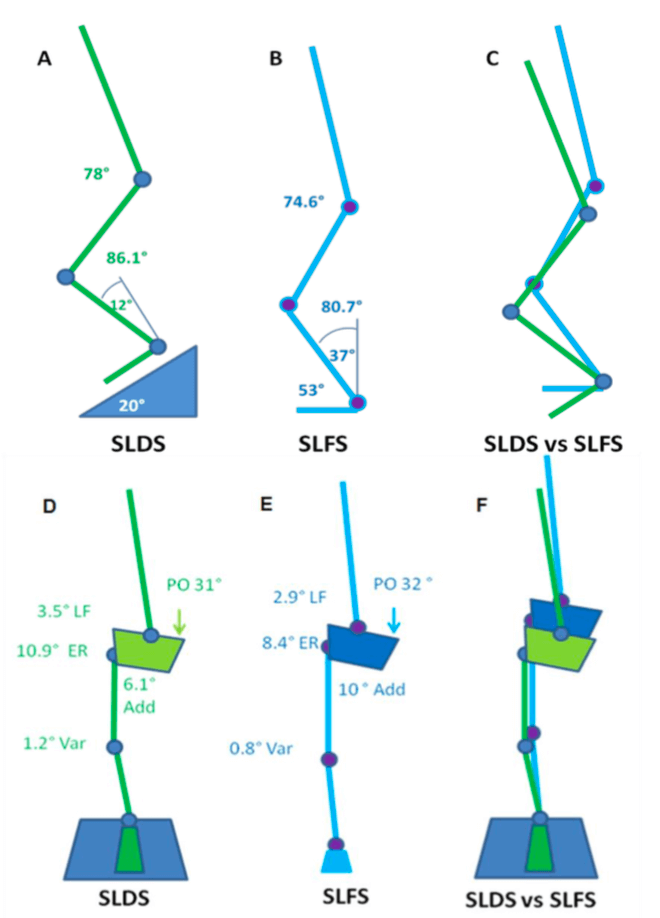
A picture tells a thousand words so in the interests of brevity, the stick squat figure is essentially a summary of two years of work.
So what this means, when someone performs a SLS on a flat surface, relative to a decline surface they tend to have:
- A more upright torso
- More rotation of the pelvis toward the weigh bearing (WB) limb
- Reduced flexion but more adduction and internal rotation of the thigh on the WB hip (pelvic close to femur)
- Less flexion of the knee but the same position relative to the foot as you look from the front (known as frontal plane knee excursion) at the bottom of range
- Reduced internal rotation of the shin
- Reduced ankle flexion
Essentially, in a flat squat you tend to ‘corkscrew’ your pelvis and adopt the medial collapse position much more easily than in the decline squat position. This may because of ankle range of motion issues as well as the ability to adequately recruit pelvic musculature. Yep – two years to get that!
STRENGTH AND MOVEMENT:
My results demonstrated a tendency for the pelvis to remain increasingly level with greater hip abduction strength. However, the relationship between strength and the pelvis was observed in the decline condition but not the flat condition. This may be due to hip abduction was shown to be significantly less (more neutral) in the SLDS which seemingly promoted greater muscle activation and subsequent control of pelvis. The self selection of squat depth may have also been a critical factor in finding as those with weak hips may have squatted deep to adopt maladaptive positions. Previous research has indicated that the hip abductors and external rotators play an important role in lower extremity alignment as they assist in the maintenance of a level pelvis [9] and are capable in balancing a number of biomechanical forces in the body [10].
Interestingly, there were no significant relationships observed between hip abduction strength and knee valgus (knee falling in) for both squatting conditions. There was however a trend between hip abduction strength and knee valgus which supported previous research. It is keeping with the assumption that increased knee valgus might also be associated with reduced hip abduction and external rotation strength [11].
SUMMARY:
- To maximise athletic function, particularly in sports such as soccer, netball and AFL, stability through the pelvis and hips, proximal lower limb, spine and abdominal structures is required [12].
- The importance of pelvis stabilisation for lower extremity injury prevention [13] particularly the knee [14-17] has been well documented in the literature.
- Adequate lumbopelvic-femur strength and muscle function may conceivably reduce exposure to other intrinsic risk factors such as inefficient force attenuation, unstable movement patterns and lower limb malalignments during activity [18, 19].
- Ankle flexibility may also be a factor in lower limb physical resilience and injury prevention.
- Support for the previous statements has been demonstrated in the relationships between hip strength measures and kinematics within selected results of my study.
There you have it. Two years of my life summarised to a few paragraphs. From a personal perspective, I took away from my research experience to be always questioning why we do things and see if there is someone out there who has answered the questions we seek. Finally, don’t overcook chicken – Ramsay doesn’t like it.
REFERENCES:
- Neely, F.G., Intrinsic risk factors for exercise-related lower limb injuries. Journal of Sports Medicine, 1998. 26(4): p. 253-263.
- Parkkari, J., U.M. Kujala, and K. Pekka, Is it possible to prevent sports injuries? Review of controlled clinical trials and recommendations for future work. Sports Medicine, 2001. 31(14): p. 985-995.
- Lysens, R.J., et al., The accident -prone and overuse-prone profiles of the young athlete. The American Journal of Sports Medicine, 1989. 17(5): p. 612-619.
- Egger, G., Sports injuries in Australia: causes, costs and prevention. A report to the national better health program., ed. C.f.H.P.a. Research. 1990, Sydney.
- Orchard, J.W. and C.F. Finch, Australia needs to follow New Zealand’s lead on sports injuries. The Medical Journal of Australia, 2002. 177: p. 38-39.
- Wu, G. and P.R. Cavanagh, ISB recommendations for standardization in the reporting of kinematic data. Journal of Biomechanics, 1995. 28: p. 1257- 1261.
- Siegal, P., R. Brackbill, and G. Heath, The epidemiology of walking exercise: implications for promoting activity among sedentary groups. American Journal of Public Health, 1995. 85(5): p. 706-710.
- Nicholl, J.P., P. Coleman, and B.T. Williams, The epidemiology of sports and exercise related injury in the United Kingdom. British Journal of Sports Medicine, 1995. 29(4): p. 232-238.
- Burnet, E.N. and P.E. Pidcoe, Isometric gluteus medius muscle torque and frontal plane pelvic motion during running. Journal of Sports Science and Medicine, 2009. 8: p. 284-288
- Niemuth, P., et al., Hip muscle weakness and overuse injuries in recreational runners. Clinical Journal of Sports Medicine, 2005. 15(1): p. 14-21.
- Hollman, J.H., et al., Relationships between knee valgus, hip-muscle strength, and hip-muscle recruitment during a single-limb step down. Journal of Sport Rehabilitation, 2009. 18: p. 104-117.
- Kibler, W.B., J. Press, and A. Sciascia, The role of core stability in the athletic function Journal of Sports Medicine, 2006. 36(3): p. 189-198.
- Leetun, D.T., et al., Core stability measures as risk factors for lower extremity injury in athletes. Medicine & Science in Sports & Exercise, 2004. 36(6): p. 926-934.
- Cichanowski, H., et al., Hip strength in collegiate female athletes with patellofemoral pain. Medicine & Science in Sport & Exercise, 2007. 39(8): p. 1227-1232.
- Ireland, M.L., et al., Hip strength measures in female with and without patellofemoral pain. Journal of Orthopaedic & Sports Physical Therapy, 2003. 33(11): p. 671-676.
- Nicholas, J.A., A.M. Strizak, and G. Veras, A study of thigh muscle weakness in different pathological states of the lower extremity. American Journal of Sports Medicine, 1976. 4: p. 241-248.
- Prins, M.R. and P.V.D. Wurff, Females with patellofemoral pain syndrome have weak hip muscles: a systematic review. Australian Journal of Physiotherapy, 2009. 55: p. 9-15.
- Willson, J.D., M.L. Ireland, and I. Davis, Core strength and lower extremity alignment during single leg squats. Medicine & Science in Sports & Exercise, 2006. 38(5): p. 945-952.
- Lee, D., The pelvic girdle: An approach to the examination and treatment of the lumbopelvic-hip region. 3rd ed. 2004, Edinburugh: Churchill Livingston.

