Shin Splints
Shin splints, known in the research as medial tibial stress syndrome (MTSS) are one of the most common running injuries we see at Praxis Physiotherapy across our Teneriffe, Buranda and Carseldine clinics.
If you’re noticing a dull ache along the inside of your shin that worsens with running, skipping or sport, you’re not alone. The good news? With the right plan, shin splints are highly manageable — and preventable.
Let’s break down what’s actually happening, why it develops, and what you can start doing today.
What Are Shin Splints (Medial Tibial Stress Syndrome)?
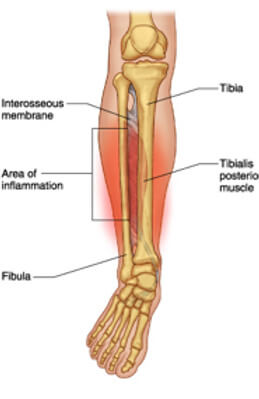
Shin splints are an overuse bone stress injury affecting the inner (medial) border of your tibia (shin bone).
What does it feel like?
Aching pain along the lower inside shin
Sharp pain when running or jumping
Tenderness to touch along the bone
Morning stiffness or pain when first starting activity
Unlike a stress fracture (which is more focal and severe), shin splints usually present as a broader area of tenderness along the bone.
What’s Actually Happening? (The Pathology Explained Simply)
MTSS is no longer thought to be just an “inflammation” problem.
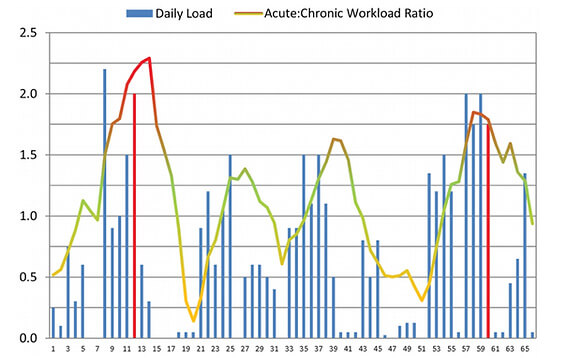
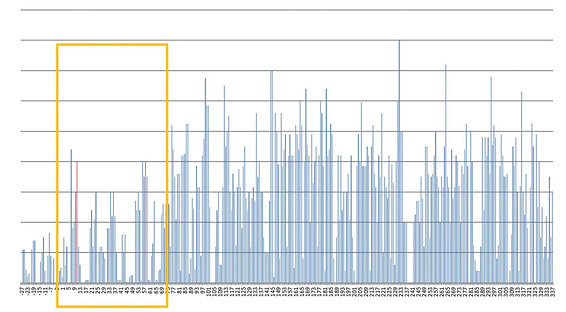
Current evidence suggests shin splints develop due to repetitive loading that exceeds the bone’s capacity to adapt. When running loads increase too quickly, the tibia experiences repeated bending stress. If recovery isn’t adequate, this leads to:
If ignored, MTSS can progress to a tibial stress fracture, which requires significantly longer time away from running.
That’s why early management matters.
Why Do Shin Splints Develop?
A large systematic review by Winkelmann et al. (2016) identified over 100 potential risk factors for MTSS, with several consistently seen in clinical practice.
Key Risk Factors Supported by Research
1. Training Load Errors
Rapid increases in running volume, intensity, or frequency are one of the strongest contributors.
(Winters et al., 2013; Nielsen et al., 2012)
2. Higher Body Mass Index (BMI)
Greater body mass increases tibial loading forces.
3. Biomechanical Factors
Increased navicular drop (foot pronation)
Greater plantarflexion range
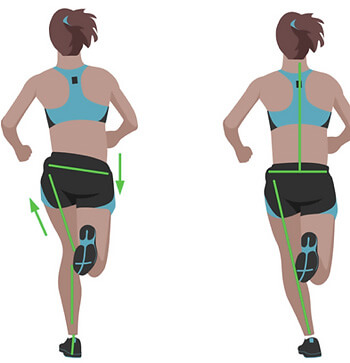
Hip muscle weakness and poor pelvic control
4. Previous History of MTSS
Recurrence risk is higher without proper rehabilitation.
Importantly flat feet alone are rarely the sole cause.
What we often see clinically is this chain reaction:
Poor hip control → knee collapses inward → foot over-pronates → increased traction stress on medial tibia.
The foot is often the victim, not the culprit.